PLEVA (Pityriasis Lichenoides et Varioliformis Acuta) is a rare, inflammatory skin disorder. It causes a sudden, rapidly changing rash that progresses from redness to blistering and crusting, potentially leaving small, pox-like scars. As the more acute and severe form within the pityriasis lichenoides spectrum, PLEVA is not contagious but its unpredictable and often symptomatic nature can cause significant physical and emotional distress, requiring careful management.
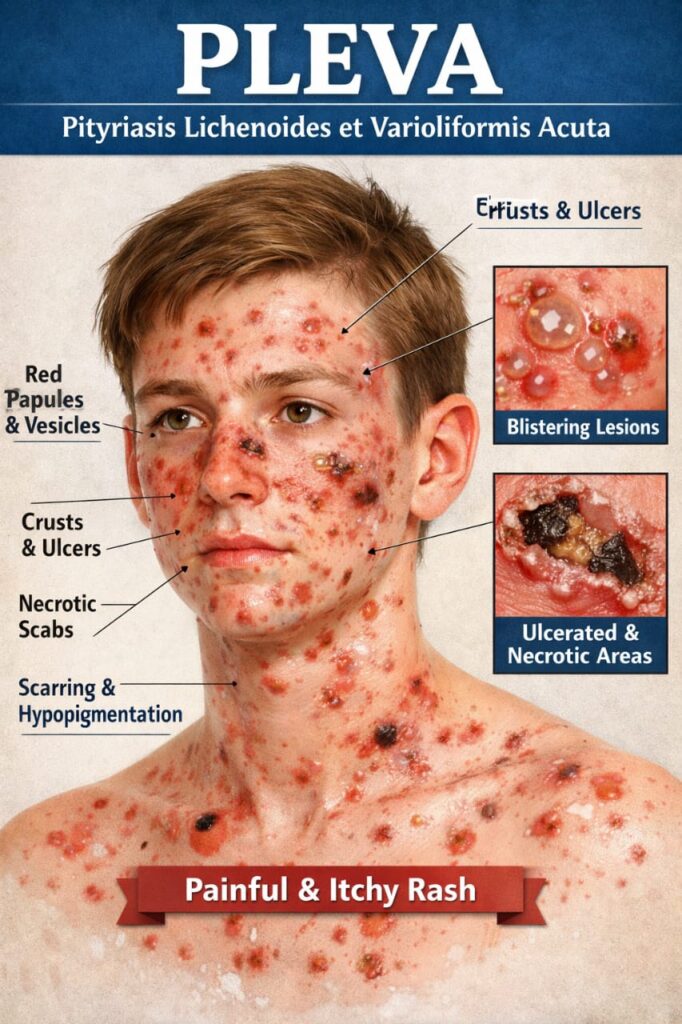
Recognizing the Symptoms of PLEVA Skin Disease
The hallmark of PLEVA skin disease is the rapid onset of lesions that can appear anywhere on the body but show a predilection for the trunk, upper arms, and thighs. The rash is often described as “cropping,” with new lesions appearing in successive waves while older ones evolve. Key symptomatic features include:
- Lesion Evolution: Individual spots typically begin as small, flat, pink-to-red macules that quickly become raised (papules). A central vesicle (small fluid-filled blister) or pustule may form, which then ruptures, crusts over, and heals. This process can result in the characteristic small, depressed, or hyperpigmented scars.
- Polymorphic Appearance: A single patient may simultaneously display red spots, blisters, crusts, and scars, creating a varied rash.
- Mild Itching or Discomfort: While sometimes asymptomatic, lesions can be mildly itchy, tender, or cause a burning sensation.
- Systemic Symptoms: In some cases, particularly in more severe or febrile forms, patients may experience low-grade fever, fatigue, headache, or joint aches accompanying the rash.
- Waxing and Waning Course: The disease is known for its unpredictable nature, with outbreaks occurring over weeks, months, or even years before potentially resolving spontaneously.
Investigating the Causes and Triggers of PLEVA Skin Disease
The exact cause of PLEVA skin disease remains unknown, which contributes to its classification as an idiopathic condition. However, prevailing medical theory suggests it is an abnormal inflammatory response, possibly triggered by an external agent in a genetically predisposed individual. Research points toward a T-cell mediated dysregulation, where the body’s own immune cells attack the skin. Several potential triggers and associations have been observed, though none are definitive:
- Infectious Triggers: Many cases are preceded by a viral or bacterial infection, such as upper respiratory infections, Epstein-Barr virus (EBV), or streptococcal infections. This has led to the hypothesis that PLEVA skin disease may represent an exaggerated, delayed immune reaction to an antigen.
- Drug Reactions: Rarely, the onset of a PLEVA-like rash has been linked to certain medications, including vaccines, antihistamines, and statins.
- Immunological Link: Its position within the pityriasis lichenoides spectrum suggests an underlying immune dysregulation, and it has been occasionally associated with other immune-mediated conditions.
- Genetic Predisposition: While not hereditary in a classic sense, certain genetic factors may influence an individual’s susceptibility to developing the condition.
Important Note: PLEVA skin disease is often a diagnosis of exclusion. Its presentation can mimic other conditions like chickenpox, guttate psoriasis, lymphomatoid papulosis, or even insect bites. Therefore, a skin biopsy is frequently essential for a definitive diagnosis. The biopsy typically shows a specific pattern of inflammatory cells invading the upper layers of the skin, helping to rule out more serious conditions.
Navigating Treatment Options for PLEVA Skin Disease
There is no universally curative treatment for PLEVA skin disease, and management strategies focus on controlling outbreaks, speeding lesion healing, relieving symptoms, and minimizing scarring. The choice of therapy depends on the patient’s age, the severity and extent of the disease, and its impact on quality of life. Common approaches include:
First-Line Topical Therapies:
- Topical Corticosteroids: Mid- to high-potency steroid creams or ointments are often used first to reduce inflammation and itching in localized disease.
- Topical Calcineurin Inhibitors: Medications like tacrolimus or pimecrolimus offer a non-steroidal option to modulate the local immune response.
- Topical Antibiotics: Erythromycin or clindamycin gels may be used for their anti-inflammatory properties, particularly if secondary bacterial infection is suspected.
Systemic Therapies (for Widespread or Resistant Cases):
- Oral Antibiotics: The mainstay of systemic treatment. Tetracyclines (e.g., doxycycline, minocycline) for adults and erythromycin for children are frequently prescribed for their anti-inflammatory effects, often leading to significant improvement within weeks.
- Phototherapy: Narrowband UVB light therapy or PUVA (psoralen plus UVA) is a highly effective option for widespread disease. The ultraviolet light helps to suppress the localized immune activity in the skin.
- Other Immunomodulators: In severe, refractory cases, dermatologists may consider systemic medications like methotrexate, dapsone, or low-dose cyclosporine to broadly dampen the immune response.
Supportive and Preventive Care:
- Emollients: Regular use of fragrance-free moisturizers helps maintain skin barrier function and soothe discomfort.
- Sun Protection: While sunlight can sometimes improve symptoms (leading to the use of phototherapy), uncontrolled sun exposure can also trigger flares in some individuals. Gentle sun protection is generally advised.
- Scar Management: Early and effective treatment of active lesions is the best way to prevent scarring. For existing scars, treatments like silicone gels, laser therapy, or microneedling may be considered after the active disease has quieted.
The prognosis for PLEVA skin disease is generally good, with many cases eventually resolving on their own over months to years, though the course can be unpredictable. Ongoing care with a dermatologist is crucial to manage flares, adjust treatments, and provide reassurance through what can be a lengthy and concerning skin journey.
