The appearance of a greenish hue on human skin is an arresting and often alarming symptom, colloquially bundled under the unsettling term green skin disease. Medically, this phenomenon is not a singular, standalone diagnosis but a dramatic presenting sign—a visual clue pointing to a diverse range of underlying conditions, from utterly benign to critically serious. Understanding what is popularly called green skin disease requires a scientific dive into dermatology, toxicology, and internal medicine to separate myth from medical reality, external stains from internal pathology.
This comprehensive guide demystifies green skin disease by exploring its multifaceted origins, outlining the systematic diagnostic pathway clinicians use, and detailing the targeted treatments that address the root cause rather than just the striking symptom.
The Causes – A Spectrum from Harmless to Critical
The green discoloration in green skin disease results from the presence of green-colored pigments in or on the skin. The origin of these pigments creates the primary categories of cause:
1. Exogenous (External) Causes: Surface Contact
This is the most frequent and least medically worrisome explanation for green skin disease. The pigment originates from an external source and stains the outer layer of the skin (stratum corneum).
- Metal Oxidation – The “Ring Stain”: The classic example is wearing jewelry made of copper or copper alloys (like brass or bronze). Acids in sweat, lotions, or soaps react with the metal, forming green copper salts (e.g., copper carbonate or copper chloride) that deposit on the skin. This is harmless, painless, and easily washed off.
- Occupational Dermatosis: Workers in constant contact with copper, nickel, or chromates—such as machinists, electroplaters, or metal sculptors—may develop persistent greenish stains on their hands and under rings or watchbands.
- Topical Products & Algae: Rarely, certain medicated creams, dyes, or even prolonged exposure to chlorinated water (with certain algae) can impart a temporary green tint.
2. Endogenous (Internal) Systemic Causes: Blood, Liver, and Metabolism
These causes are medically significant, as the green color arises from within the body due to a biochemical or circulatory disorder.
- Hemoglobin Derivatives – The “Bronze-Green” Hue: In severe, chronic hemolytic anemias (where red blood cells break down rapidly), the body may produce unusual breakdown products of hemoglobin. Sulfhemoglobinemia or methemoglobinemia, often drug-induced, can cause skin to appear a unique slate-gray, cyanotic blue, or even a greenish-brown “bronze.” This is a sign of significant blood oxygen transport impairment.
- Cholestatic Jaundice with a Green Cast: In long-standing obstructive jaundice (e.g., from advanced bile duct blockage), the classic yellow bilirubin pigment can undergo oxidation in the skin over time, mixing to produce a subtle greenish-yellow tint. This signals advanced liver or biliary disease.
- Hypercupremia: While Wilson’s disease (genetic copper overload) famously causes brown Kayser-Fleischer rings in the eyes, profound, acute copper toxicity is a theoretical—though extremely rare—cause of systemic discoloration.
3. Infectious & Biological Causes:
- Pseudomonas aeruginosa Infection – A Medical Emergency: This bacterium produces vibrant green pigments (pyocyanin and pyoverdine). In severe cases—such as in burn wound infections, folliculitis from hot tubs, or the life-threatening condition echyma gangrenosum in immunocompromised patients—the wound bed, pus, or necrotic skin can exhibit a vivid, ominous green-blue discoloration. This is a critical sign requiring immediate intervention.
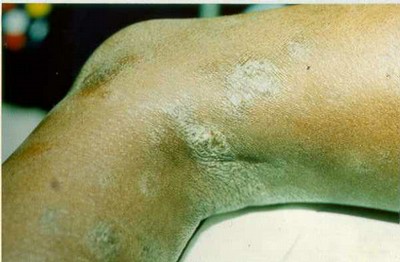
- Alkaptonuria (Ochronosis) – The Genetic Cause: A rare autosomal recessive disorder where the body lacks the enzyme to metabolize homogentisic acid. Over decades, this acid oxidizes and binds to collagen in connective tissues. This leads to ochronosis: a bluish-gray or greenish-black pigmentation in cartilage (ears, nose), sclerae (whites of the eyes), and skin over tendons and joints. It is progressive and associated with severe arthritis.
The Diagnosis – The Clinical Detective Work
Diagnosing the cause of green skin disease is a methodical process that moves from the simplest explanation to the more complex. A dermatologist or internist will act as a detective, following a standard protocol:
Step 1: Comprehensive Patient History
Key questions help narrow the field:
- Onset & Pattern: Did it appear suddenly or gradually? Is it under a ring/watch (local) or on the face/trunk (generalized)?
- Occupational & Personal Habits: Do you work with metals, chemicals, or dyes? Do you wear copper jewelry or use new topical products?
- Associated Symptoms: Is there pain, fever, itching, fatigue, joint pain, or jaundice? Symptoms point to systemic or infectious causes.
- Medical & Medication History: Any known liver, blood, or genetic disorders? Use of sulfonamides, nitrates, or other drugs linked to blood pigment changes?
Step 2: Detailed Physical Examination
The physician will assess:
- Color Quality: Is it a bright, superficial green (suggesting external stain) or a deep, dusky greenish-bronze (suggesting blood or metabolic cause)?
- Distribution & Wipe Test: Crucially, they will attempt to wipe the area with an alcohol swab or soapy gauze. If the green comes off, an external cause is confirmed.
- Associated Signs: Checking for scleral color (jaundice), Kayser-Fleischer rings (Wilson’s), skin breakdown/wounds (infection), or joint deformities (alkaptonuria).
Step 3: Targeted Diagnostic Testing
Based on history and exam, specific tests are ordered:
- For Suspected External Cause: The wipe test is often diagnostic. No further testing is needed if it resolves with cleansing and avoidance.
- For Suspected Internal/Systemic Cause:
- Blood Tests: A complete metabolic panel is essential.
- Complete Blood Count (CBC) & Reticulocyte Count: To detect hemolytic anemia.
- Liver Function Tests (LFTs), Bilirubin (Direct/Indirect): To assess for cholestasis or liver disease.
- Ceruloplasmin & Serum Copper: To screen for Wilson’s disease.
- Blood Gas with Co-oximetry: Can definitively diagnose methemoglobinemia or sulfhemoglobinemia.
- Microbiological Culture: Any green-tinged wound exudate must be cultured to identify Pseudomonas aeruginosa or other pathogens.
- Urine Analysis: For alkaptonuria, a fresh urine sample may appear normal but turns dark brown or black upon standing or alkalization due to homogentisic acid oxidation.
- Skin Biopsy: A punch biopsy, examined under a microscope with special stains, can reveal pigment deposits (like in ochronosis) within the dermis, confirming an internal origin.
- Blood Tests: A complete metabolic panel is essential.
The Treatment – Addressing the Source
Treatment for green skin disease is 100% cause-dependent. The goal is to eliminate the source of the green pigment.
For External Causes:
- Cleansing & Prevention: Thorough washing with soap and water or a weak acid (like lemon juice or vinegar) removes copper salts. Prevention involves creating a barrier: apply clear nail polish to the inside of jewelry, wear protective gloves, or switch to hypoallergenic metals.
For Internal Blood & Metabolic Causes:
- Treating the Underlying Disorder:
- Hemolytic Anemias & Blood Pigment Disorders: Treatment may involve discontinuing offending drugs, administering methylene blue (for methemoglobinemia), or managing the underlying anemia with medications or supplements.
- Cholestatic Liver Disease: Requires management of the biliary obstruction (via ERCP or surgery) or treatment of the liver disease itself (e.g., ursodeoxycholic acid for PBC). Resolving the cholestasis will gradually clear the jaundice and any greenish tint.
- Wilson’s Disease: Lifelong chelation therapy (e.g., with D-penicillamine or trientine) to remove excess copper.
- Alkaptonuria: While no cure exists, treatment focuses on symptom management. A low-protein diet (specifically low in phenylalanine and tyrosine) and medication like nitisinone can significantly reduce the production of homogentisic acid, potentially slowing pigment deposition and disease progression. Pain management for associated arthritis is crucial.
For Infectious Causes:
- Pseudomonas Infection: This requires urgent, aggressive treatment. Therapy involves:
- Debridement: Surgical removal of infected, necrotic tissue.
- Targeted Antibiotics: Based on culture sensitivities, typically intravenous anti-pseudomonal agents like ceftazidime, ciprofloxacin, or piperacillin-tazobactam.
- Topical Antiseptics: For wound care (e.g., acetic acid soaks, silver sulfadiazine cream).
Conclusion: A Symptom Demanding Respect
The phenomenon known as green skin disease powerfully illustrates a core tenet of medicine: the skin is a highly visible diagnostic canvas. Dismissing a green discoloration as merely odd can be a dangerous mistake, as it may be the sole early sign of a severe Pseudomonas sepsis in a vulnerable patient or the visible tip of a complex metabolic disorder like alkaptonuria.
Conversely, panicking over a simple copper stain from a ring is unnecessary. The key is informed assessment. If the discoloration is persistent, widespread, associated with any systemic symptoms, or centered on a wound, immediate medical consultation is non-negotiable. Through a careful history, a simple wipe test, and targeted diagnostics, the true cause of green skin disease can be uncovered, allowing for precise treatment that addresses the root problem, resolves the alarming symptom, and safeguards the patient’s health.