Heart disease screening is the proactive process of checking for cardiovascular disease and its risk factors in individuals who do not yet show symptoms. This foundational practice of preventive medicine operates on a powerful, evidence-based principle: identifying and managing risks early can dramatically alter a person’s health trajectory. Early detection through systematic heart disease screening allows for interventions that can slow, stop, or even reverse the progression of conditions like coronary artery disease, often preventing catastrophic events like heart attacks and strokes. It transforms heart health from a reactive model—treating emergencies—to a proactive strategy focused on preservation and longevity.

Why Heart Disease Screening is Critical
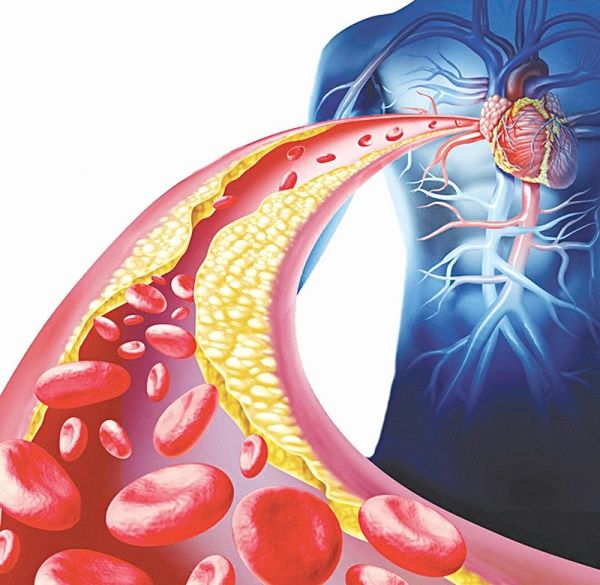
Cardiovascular disease often develops silently for decades. Plaque can accumulate in arteries (atherosclerosis) without causing any chest pain or shortness of breath—until a sudden blockage occurs. Heart disease screening aims to unveil this silent progression. Its core purpose is twofold: to assess an individual’s overall risk and to detect subclinical disease. By measuring key biomarkers and using non-invasive tests, screening provides a personalized risk profile. This profile guides everything from lifestyle counseling to the decision to start preventive medications like statins or aspirin. Ultimately, the goal of heart disease screening is not just to add years to life, but to add life to years by maintaining cardiac function and preventing disability.
Who Needs Heart Disease Screening and When?
Guidelines for heart disease screening are not one-size-fits-all; they are based on age, family history, and established risk factors. For most adults, the formal assessment of cardiovascular risk should begin at age 20, with regular check-ins on key metrics like blood pressure and cholesterol.
However, the intensity and tools used in heart disease screening change as risk increases. Key groups who should undergo more thorough or earlier screening include:
- Adults over 40: Risk increases significantly with age.
- Individuals with a family history of early heart disease (e.g., a father or brother diagnosed before age 55, or a mother or sister before age 65).
- People with established risk factors, including hypertension, high cholesterol, diabetes, obesity, or a smoking habit.
- Anyone planning to start a vigorous exercise program, to ensure safety.
- People with conditions linked to heart disease, such as chronic kidney disease or certain inflammatory disorders.
The Heart Disease Screening Toolkit: From Basic to Advanced
A comprehensive heart disease screening protocol is tiered, starting with simple, in-office assessments and progressing to more advanced imaging only when warranted.
Tier 1: The Foundational Clinical Assessment (For Everyone)
This is the essential first step in any heart disease screening and is performed during a routine physical:
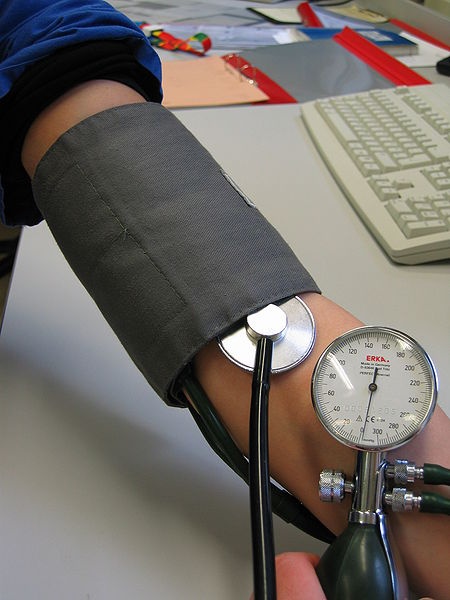
Blood Pressure Measurement: Hypertension is a leading risk factor and is often asymptomatic.
Body Mass Index (BMI) & Waist Circumference: Measures of obesity, a major contributor to metabolic syndrome.

Fasting Blood Glucose or Hemoglobin A1c: Screens for prediabetes and diabetes.

- Fasting Lipoprotein Panel: The critical cholesterol test that measures total cholesterol, LDL (“bad”) cholesterol, HDL (“good”) cholesterol, and triglycerides.
- Thorough History: A discussion of diet, physical activity, smoking status, and family history of heart disease.
The data from this initial tier is often used to calculate a 10-year Atherosclerotic Cardiovascular Disease (ASCVD) Risk Score, a powerful tool that quantifies an individual’s chance of having a heart attack or stroke in the next decade.
Tier 2: Advanced Screening (For Intermediate or High Risk)
When the foundational assessment suggests elevated risk, the following tools can provide greater clarity:
Electrocardiogram (ECG/EKG): A simple test that records the heart’s electrical activity. It can detect signs of a prior, silent heart attack, arrhythmias, or other abnormalities.
Coronary Artery Calcium (CAC) Scan: This is a pivotal advanced screening tool. A non-contrast CT scan detects and quantifies calcium deposits in the coronary arteries. A CAC score of zero indicates very low near-term risk, while a high score confirms the presence of atherosclerosis and can strongly guide decisions about statin therapy.
Ankle-Brachial Index (ABI): A simple blood pressure comparison between the arm and ankle that screens for Peripheral Artery Disease (PAD), a strong marker for systemic atherosclerosis.

Understanding Your Results and Taking Action
The results of heart disease screening should lead to a clear, personalized action plan developed with your doctor.
- Low Risk: A reassuring result. The focus remains on maintaining a heart-healthy lifestyle (the “Life’s Essential 8” from the American Heart Association), with repeat screening every 4-5 years.
- Intermediate Risk: This is where personalized medicine comes into play. A doctor may use a tool like the CAC scan to “reclassify” risk up or down. The decision to begin medication is made based on this refined risk assessment and patient preference.
- High Risk: This result is a clear call to action. It typically involves initiating both intensive lifestyle therapy and medications (e.g., statins, blood pressure drugs) to aggressively lower risk.
Important Consideration: Heart disease screening is a powerful tool, but it is not without potential downsides, such as false-positive results leading to anxiety or unnecessary follow-up procedures. This is why it is most valuable when applied selectively based on guidelines, not universally for every person. A conversation with a healthcare provider is essential to weigh individual benefits and potential harms.
The Bottom Line: Empowerment Through Proactivity
Heart disease screening is more than just a set of tests; it is an empowering strategy that puts individuals in control of their heart health. By moving from uncertainty to a clear understanding of personal risk, people can make informed decisions in partnership with their doctors. This proactive path, illuminated by the insights gained from heart disease screening, is the most effective way to prevent the world’s leading cause of death and ensure a longer, healthier, and more vibrant life. The first step is as simple as scheduling a visit to discuss a screening plan with your primary care physician.
