Herpes skin disease is a common yet often stigmatized group of viral infections, including cold sores, genital herpes, and shingles, all characterized by painful, recurrent blisters. Caused by the Herpesviridae family of viruses, it affects millions worldwide. While the diagnosis can be daunting, herpes skin disease is highly manageable. With proper education, medical treatment, and lifestyle changes, individuals can control symptoms, reduce outbreaks, and lead full, healthy lives. This guide provides a complete overview of its symptoms, transmission, and care.

Understanding Herpes Skin Disease: The Viral Culprits and How They Spread
At the core of herpes skin disease are neurotropic viruses—viruses that infect nerve cells. After the initial (primary) infection, these viruses travel along sensory nerves to establish a permanent, latent (dormant) residency in nerve cell clusters called ganglia. They can later reactivate, traveling back down the nerve to the skin’s surface, causing recurrent outbreaks, often triggered by stress, illness, or immune suppression.
The primary viruses responsible for cutaneous manifestations are:
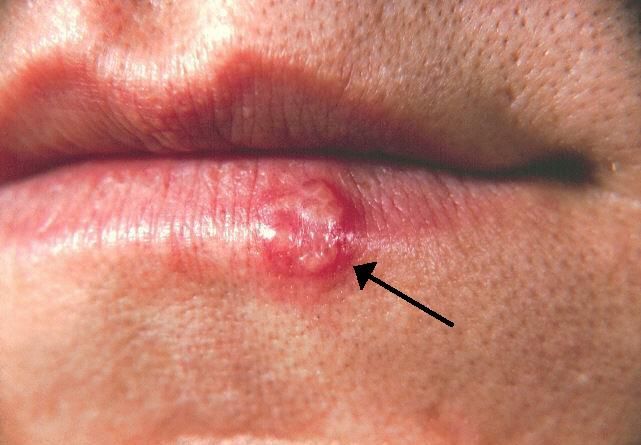
- Herpes Simplex Virus Type 1 (HSV-1): Historically labeled “oral herpes,” HSV-1 is traditionally associated with cold sores or fever blisters around the lips and mouth (herpes labialis). However, it is a common cause of genital herpes through oral-genital contact. It can also cause herpetic whitlow (painful finger infection) and herpes gladiatorum (skin infections in athletes).
- Herpes Simplex Virus Type 2 (HSV-2): This strain is the classic cause of genital herpes, characterized by blistering sores on or around the genitals, rectum, and thighs. Like HSV-1, it establishes latency and can recur.
- Varicella-Zoster Virus (VZV): This single virus causes two distinct clinical presentations of herpes skin disease:
- Chickenpox (Varicella): The widespread, itchy, blistering rash of the initial primary infection, usually in childhood.
- Shingles (Herpes Zoster): A localized, often excruciatingly painful blistering rash that occurs when the dormant VZV reactivates decades later. The rash typically follows a single sensory nerve pathway (a dermatome), appearing as a stripe of blisters on one side of the torso or face.
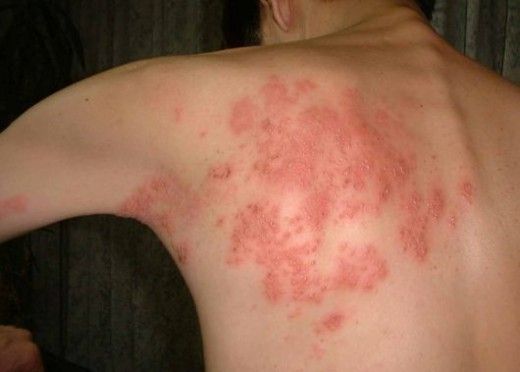
Transmission of Herpes Skin Disease:
Understanding transmission is key to prevention. Herpes skin disease is highly contagious, primarily through direct skin-to-skin contact with an active lesion or, critically, via “asymptomatic viral shedding,” where the virus is present on the skin without visible sores.
- HSV-1 & HSV-2: Spread via contact with infected saliva, genital secretions, or the fluid from herpes sores. This can occur through kissing, oral sex, vaginal sex, anal sex, or even touching a sore and then touching another part of the body (auto-inoculation).
- VZV: Chickenpox is spread through airborne respiratory droplets (coughing, sneezing) or direct contact with blister fluid. Shingles itself is not airborne; it is spread only through direct contact with the fluid from active shingles blisters, which can then cause chickenpox in a non-immune person.
Recognizing the Symptoms: From Prodrome to Healing
Symptoms of herpes skin disease vary based on the virus, whether it’s a first episode or a recurrence, and the individual’s immune status. However, most outbreaks follow a predictable pattern.
1. The Prodromal Phase (Warning Signs):
Before any blisters appear, many people experience a prodrome—subtle sensations at the site where the outbreak will occur. This can include:
- Tingling, itching, or burning
- Pain, tenderness, or sensitivity
- Aching or shooting pains in the legs, hips, or buttocks (common with genital herpes)
- For shingles, the prodromal pain can be severe and mistaken for other conditions like heart or kidney problems.
2. The Active Outbreak:
This is the classic symptomatic phase of herpes skin disease.
- Cluster of Lesions: Small, painful, fluid-filled blisters (vesicles) appear in crops or clusters on a red, inflamed base of skin.
- Ulceration and Crusting: The fragile blisters break open within a few days, leaving shallow, moist, painful open sores (ulcers). These ulcers eventually dry out and form a yellow or brown crust as they heal. Healing usually occurs within 2-4 weeks for a primary outbreak and more quickly for recurrences, typically without scarring if left undisturbed.
3. Associated Systemic Symptoms:
Especially during a severe primary infection, individuals may experience:
- Fever and chills
- Swollen and tender lymph nodes near the outbreak site
- Muscle aches, headache, and fatigue
- Pain or difficulty urinating (with genital herpes)
Specific Presentations by Type:
- Oral Herpes (HSV-1): Blisters on the lips, gums, tongue, and inside of the cheeks. Gums may become swollen and bleed.
- Genital Herpes (HSV-1/2): Sores on the penis, scrotum, vulva, vagina, cervix, buttocks, anus, or thighs. The first outbreak is often the most severe.
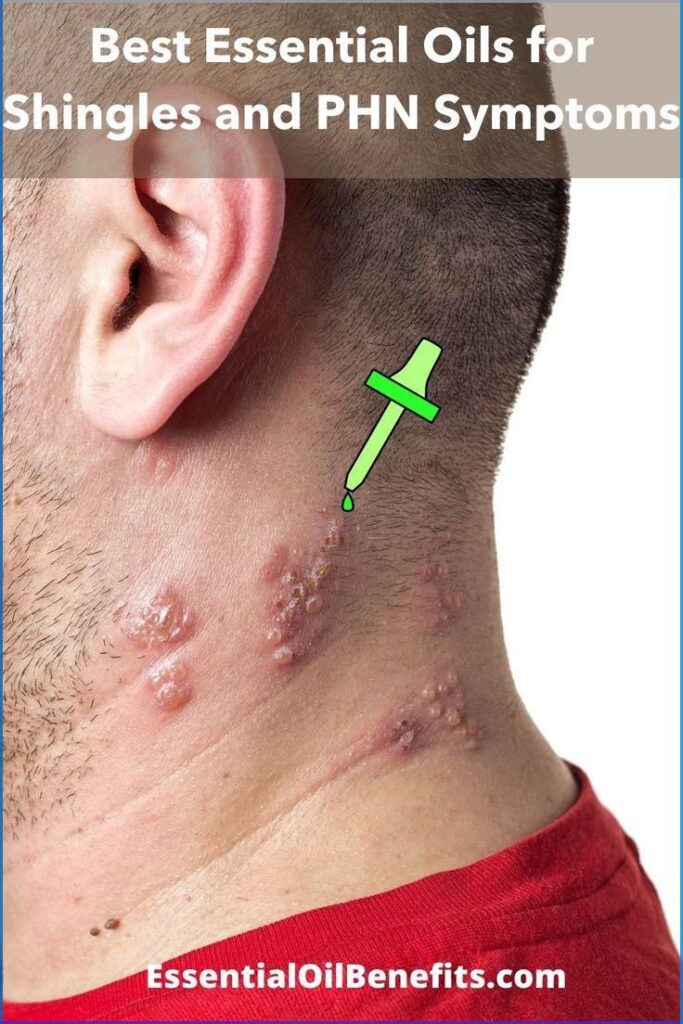
- Shingles (Herpes Zoster): A painful, burning, or tingling rash limited to one side of the body, following a dermatomal band. Common sites are the torso, face (potentially affecting the eye—herpes zoster ophthalmicus, a medical emergency), and neck. The major complication is postherpetic neuralgia (PHN), debilitating nerve pain that persists for months or years after the rash has healed.
A Complete Care Guide: Diagnosis, Treatment, and Proactive Management
Diagnosis:
An accurate diagnosis is the foundation of effective management for herpes skin disease. Methods include:
- Viral Culture: Swab of fluid from a fresh blister. Best if done within 48-72 hours of blister appearance.
- PCR (Polymerase Chain Reaction) Test: A highly sensitive swab test that detects viral DNA, preferred over culture for its accuracy.
- Blood Tests (Type-Specific Serology): Detect IgG antibodies to HSV-1 or HSV-2. These tests indicate a past or present infection and are useful when no active sores are present, for diagnosis of asymptomatic individuals, or for couples wanting to understand their status.
Medical Treatment:
While there is no cure to eliminate the virus from the body, antiviral medications are highly effective in managing herpes skin disease.
- Episodic Therapy: Taking antiviral pills (e.g., acyclovir, valacyclovir, famciclovir) at the first sign of prodrome or an outbreak can shorten its duration, reduce severity, and accelerate healing.
- Suppressive Therapy: For individuals with frequent or severe recurrences (e.g., more than 6 per year), taking a daily low-dose antiviral can suppress viral activity, reducing outbreak frequency by 70-80% and lowering the risk of transmission to partners.
- Shingles-Specific Care: Prompt antiviral treatment within 72 hours of rash onset is critical to reduce acute pain, complication risk, and PHN development. PHN itself is managed with medications like gabapentin, pregabalin, or topical lidocaine patches.
Self-Care and Symptom Relief:
- Pain Management: Use OTC pain relievers (ibuprofen, acetaminophen). For genital sores, urinating in a bath of warm water or using a squeeze bottle to pour water over the area can reduce stinging.
- Skin Care: Keep lesions clean and dry to prevent bacterial infection. Gently wash with mild soap and water. Apply cool, wet compresses for 20 minutes several times a day to soothe pain and inflammation.
- Comfort Measures: Wear loose-fitting, breathable cotton clothing. Avoid picking or scratching sores.
Prevention and Lifestyle Strategy:

- Vaccination: The Shingrix vaccine is >90% effective at preventing shingles and PHN and is recommended for healthy adults 50+. The chickenpox vaccine prevents primary VZV infection.
- Communication and Safer Practices: Open communication with partners is vital. Using condoms or dental dams reduces—but does not eliminate—transmission risk, as the virus can shed from skin not covered by the barrier. Avoid all skin-to-skin contact in the affected area during prodromal symptoms and active outbreaks.
- Trigger Management: Identify and mitigate personal triggers. Common ones include emotional or physical stress, illness/fever, fatigue, hormonal changes (e.g., menstruation), surgical trauma, and ultraviolet light (for oral herpes—use lip balm with SPF).
Conclusion
Navigating life with herpes skin disease is a journey of education, proactive healthcare, and self-compassion. The condition, while chronic, does not define a person’s health or worth. By recognizing the diverse symptoms—from the initial prodromal tingling to the distinctive blister clusters—and engaging with a complete care plan that includes accurate diagnosis, effective antiviral therapy, thoughtful self-care, and preventive strategies, the impact of herpes skin disease can be profoundly minimized. If you suspect you have symptoms, seek a confirmed diagnosis from a healthcare provider. With knowledge as your tool and modern medicine as your support, you can take confident control of your health and well-being.
