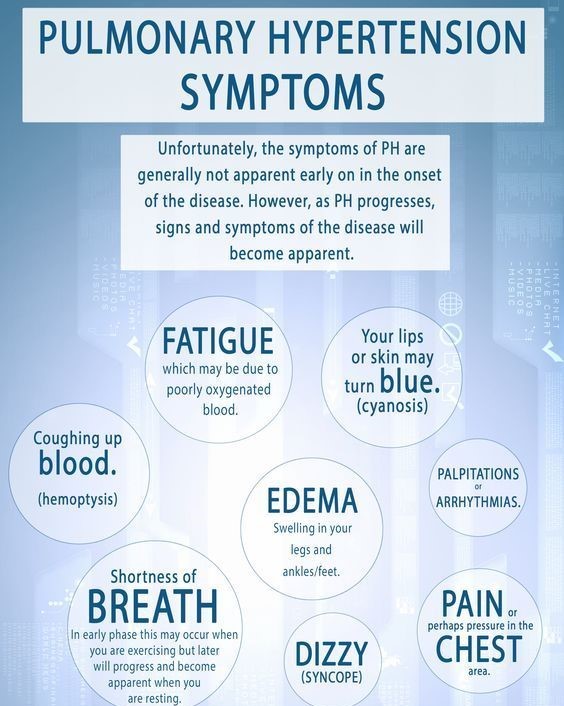
Pulmonary hypertension Medications (PH) is high blood pressure in the arteries that carry blood from the heart to the lungs. Its medications are specifically designed to dilate (widen) these narrowed arteries, reduce strain on the heart, and slow disease progression.
Unlike common high blood pressure treatments, pulmonary hypertension medication targets unique pathways in the lung’s blood vessels. Treatment is tailored to the specific type and severity of PH.
Main Classes of Pulmonary Hypertension Medication
- Vasodilators (Dilate Lung Arteries)
- PDE-5 Inhibitors: Sildenafil, Tadalafil. Increase blood flow by relaxing artery walls.
- Soluble Guanylate Cyclase (sGC) Stimulators: Riociguat. Also promotes artery relaxation.
- Endothelin Receptor Antagonists (ERAs)
- Bosentan, Ambrisentan, Macitentan.
- Action: Block endothelin, a substance that causes blood vessels to narrow.
- Prostacyclin Pathway Medications
- Prostacyclin Analogues: Epoprostenol (IV), Treprostinil (IV, SC, inhaled), Iloprost (inhaled).
- Action: Mimic prostacyclin, a substance that dilates blood vessels and prevents clotting. These are often crucial for advanced PH.
- Combination Therapy
- Most patients eventually use two or more classes of pulmonary hypertension medication from different pathways to achieve better control.
Important Considerations
- Targeted Treatment: These drugs are primarily for Group 1: Pulmonary Arterial Hypertension (PAH). They are not typically used for PH caused by left heart disease or lung disease (Groups 2 & 3).
- Specialist-Driven: Treatment is complex and must be managed by a PH specialist. Dosing and delivery methods (oral, inhaled, intravenous) are highly individualized.
- Contrast with Asthma Care: Unlike asthma inhalers that target airway inflammation, pulmonary hypertension medication works directly on the lung’s vascular system. Patients with both conditions require very careful, coordinated care by specialists.
Always adhere strictly to your prescribed regimen and report any side effects to your healthcare team immediately.
Side Effects of Pulmonary Hypertension Medications
While essential for managing pulmonary arterial hypertension (PAH), these powerful medications can cause significant side effects that require careful monitoring.
Common Class-Specific Side Effects:
- Endothelin Receptor Antagonitors (ERAs): Liver enzyme elevation, fluid retention, anemia.
- PDE-5 Inhibitors (e.g., sildenafil): Headache, flushing, dizziness, nasal congestion, visual disturbances.
- Prostacyclins: Jaw pain, flushing, diarrhea, nausea, rash, hemoptysis (coughing up blood).
Key Risks & Comorbidities:
- Systemic Hypotension: Vasodilatory effects can lower overall blood pressure. This is particularly critical in patients with hypotension heart failure (especially heart failure with reduced ejection fraction), as it can worsen organ perfusion. It is also a major concern in hypotension in pregnancy, requiring extreme caution and specialist management.
- Hemoptysis: Coughing up blood is a serious potential side effect, notably with prostacyclins. In clinical coding, hemoptysis ICD 10 is tracked under code R04.2. This symptom must be urgently evaluated, as it can indicate disease progression or complications. For patients with underlying hemoptysis bronchiectasis, the risk may be increased, requiring a careful risk-benefit assessment.
Important Note:
The presence of side effects is not always a reason to stop therapy. Management often involves dose adjustment, treating the symptom, or switching medications. Any new or worsening symptom must be reported immediately to your PH specialist. Never adjust your medication regimen without direct medical supervision.
Managing pulmonary hypertension medication
Effective pulmonary hypertension management requires a structured, lifelong approach coordinated by a specialist. Proper medication management is its cornerstone, going beyond simply taking prescriptions.
Core Principles of Management
- Structured Care Plan: Every patient needs an individualized Pulmonary hypertension care plan. This plan details medication schedules, monitoring protocols, lifestyle modifications, and emergency instructions.
- Adherence is Critical: Pulmonary hypertension medication must be taken exactly as prescribed, especially for continuous intravenous (IV) or subcutaneous therapies. Even minor deviations can lead to clinical deterioration.
- Regular Monitoring & Titration: Patients undergo frequent tests (echocardiograms, 6-minute walk tests, blood work) to assess response. Dosages are carefully adjusted (“titrated”) over time, often upward, to maintain efficacy.
- Combination Therapy: Most patients progress to combination therapy—using two or more drug classes from different pathways (e.g., an ERA plus a PDE-5 inhibitor). This approach is more effective than single-drug therapy for many.
Advanced and Evolving Options
The landscape of Pulmonary hypertension treatment options is expanding. This now includes:
- Novel drug formulations for easier administration.
- Research into personalized medicine based on genetics and biomarkers.
- Important Note on Novel Combinations: Research is exploring combinations with drugs from other fields. For example, Keytruda combination therapy (referring to the immunotherapy pembrolizumab) is being studied in specific cancer-related PH contexts but is not a standard treatment for PAH. Such advanced protocols are strictly confined to clinical trials under specialist supervision.
Holistic Management
Medication is one pillar of pulmonary hypertension management. A complete plan also includes:
- Supportive Care: Diuretics for fluid overload, oxygen therapy, and anticoagulation in select cases.
- Lifestyle: Supervised rehabilitation, a low-sodium diet, and avoiding pregnancy.
- Surgical Options: For eligible patients, this may include atrial septostomy or lung transplantation.
Conclusion: Successful management hinges on a strong partnership between the patient and the PH care team, meticulous adherence to the personalized Pulmonary hypertension care plan, and proactive communication about any changes in symptoms or side effects.
Side Effects of Pulmonary Hypertension Medications
Managing side effects is a crucial part of pulmonary hypertension medication therapy. Common side effects vary by drug class but often result from their potent vasodilatory effects.
Common Medication-Specific Side Effects
- PDE-5 Inhibitors (e.g., sildenafil): Headache, flushing, nasal congestion, dizziness.
- Endothelin Receptor Antagonists (ERAs): Swelling (edema), potential liver enzyme changes, anemia.
- Prostacyclin Analogues: Jaw pain, nausea, diarrhea, skin rash, and flushing.
Managing Side Effects and Complications
- Cough: A common complaint that requires careful evaluation. It can be a side effect of the medication itself, a symptom of disease progression, or an unrelated issue like cough from allergies. Simple remedies like cough lozenges may soothe an irritated throat but do not treat the underlying cause. Note: Any new, worsening, or persistent cough must be reported to your PH specialist.
- Severe Side Effects: A rigorous pharmaceutical risk assessment is conducted by your care team before and during treatment to balance benefits against serious risks. This is vital for preventing or managing severe reactions, including a rare but serious event like cough syncope (fainting triggered by a coughing spell, which can indicate significant cardiovascular strain).
Critical Patient Guidance
Always report side effects to your healthcare team. Do not stop or adjust your medication on your own, as this can be dangerous. Your doctor may manage side effects by adjusting the dose, changing the timing of administration, or prescribing additional supportive treatments.