A rare autoimmune disease affecting lungs occurs when the body’s immune system mistakenly attacks healthy lung tissue, leading to inflammation, scarring (fibrosis), and impaired breathing. Unlike more common lung conditions, these disorders are systemic, often involving other organs as well.
Common Symptoms
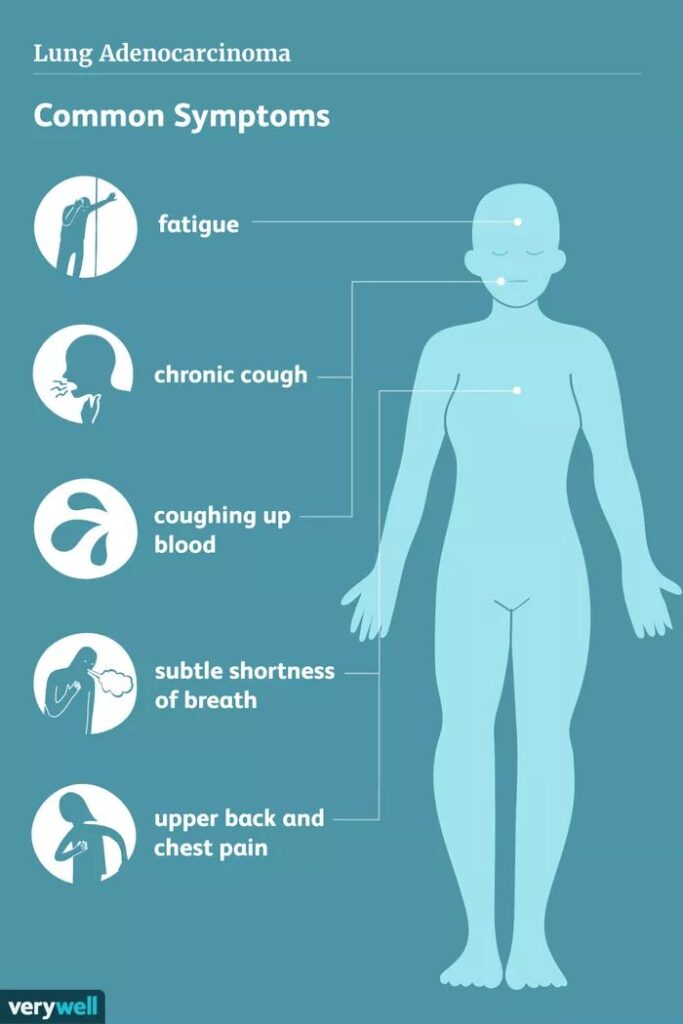
Symptoms can be progressive and often mimic other lung diseases, including:
- Persistent dry cough
- Shortness of breath (dyspnea), especially during activity
- Fatigue and general weakness
- Chest discomfort or pain
- Unexplained fever or weight loss (in systemic cases)
- Clubbing of fingers (in advanced stages)
Major Types
Several rare autoimmune disease affecting lungs fall under this category, including:
- Interstitial Lung Disease (ILD) associated with connective tissue diseases (e.g., Rheumatoid Arthritis-ILD, Scleroderma-ILD).
- Granulomatosis with Polyangiitis (GPA): Causes inflammation of blood vessels, forming granulomas in the lungs and airways.
- Sarcoidosis: Characterized by the growth of tiny granulomas, most commonly in the lungs and lymph nodes.
- Eosinophilic Granulomatosis with Polyangiitis (EGPA): Involves asthma, high eosinophil count, and lung inflammation.
- Autoimmune Pulmonary Alveolar Proteinosis (aPAP): A disorder where surfactant builds up excessively in the lung’s air sacs.
Diagnosis and Treatment
Diagnosis requires a multidisciplinary approach, often involving:
- Imaging: High-Resolution CT (HRCT) scans to visualize lung patterns.
- Blood Tests: To detect specific autoimmune antibodies (e.g., ANCA, ANA).
- Lung Function Tests (PFTs): To assess breathing capacity.
- Biopsy: In some cases, a lung or other tissue biopsy is needed for confirmation.
Treatment aims to suppress the abnormal immune response and preserve lung function:
- Immunosuppressants: Corticosteroids (e.g., prednisone), mycophenolate, azathioprine, or cyclophosphamide.
- Biologic Therapies: Rituximab for certain vasculitides.
- Antifibrotic Drugs: Such as nintedanib or pirfenidone for progressive lung scarring.
- Supportive Care: Oxygen therapy, pulmonary rehabilitation, and vaccination against respiratory infections.
- Lung Transplant: Considered in severe, end-stage disease.
Key Takeaway
Early recognition of a rare autoimmune disease affecting lungs is critical. While these conditions are chronic, prompt diagnosis and tailored treatment can significantly slow progression, manage symptoms, and improve quality of life. Collaboration with a rheumatologist and pulmonologist is essential for effective care.
Navigating a Rare Autoimmune Disease Affecting Lungs
Receiving a diagnosis of a rare autoimmune disease affecting lungs, such as interstitial lung disease (ILD) leading to pulmonary fibrosis, can be overwhelming. This journey involves understanding your specific diagnosis, its progression, and a multi-faceted treatment plan. Here’s a brief guide to key areas you’ll encounter.
1. Understanding Your Diagnosis & Coding
Your medical team will classify your condition for records and insurance. A common code used is pulmonary fibrosis icd 10, often J84.10 (for unspecified pulmonary fibrosis) or more specific codes like J84.112 (Idiopathic Pulmonary Fibrosis). This precise coding is crucial for your care coordination and pulmonary fibrosis treatment approvals.
2. Tracking Disease Progression: The Stages
Understanding the pulmonary fibrosis stages helps gauge the disease’s impact and guide therapy. Staging typically considers:
- Mild: Minimal symptoms, often only with exertion; mild changes on CT scan.
- Moderate: Noticeable shortness of breath, reduced lung function on tests.
- Severe: Significant oxygen need, major decline in lung function, greatly reduced activity tolerance.
Regular pulmonary function tests and imaging help monitor these pulmonary fibrosis stages.
3. Exploring Treatment Avenues
A comprehensive pulmonary fibrosis treatment plan is personalized and may include:
- Anti-fibrotic Medications: Drugs like nintedanib or pirfenidone to slow scarring.
- Immunosuppressants: To dampen the underlying autoimmune attack (e.g., corticosteroids, mycophenolate).
- Oxygen Therapy: To relieve breathlessness and protect the heart.
- Pulmonary Rehabilitation: A supervised program to improve strength and breathing techniques.
4. Investigating Adjunctive Therapies
Patients often research supportive options to improve quality of life. Some inquire about hyperbaric oxygen therapy near me. While HBOT is not a standard treatment for pulmonary fibrosis and is primarily used for different conditions (like non-healing wounds), some seek it for its potential theoretical benefits in reducing inflammation. It is critical to discuss any adjunctive therapy with your specialist before proceeding, as evidence for its efficacy in autoimmune lung fibrosis is limited.
Navigating Forward
Successfully navigating this path relies on a strong partnership with a specialized care team, typically including a pulmonologist and rheumatologist. Stay informed, advocate for yourself, and utilize support networks to manage this complex condition.
Living with a Rare autoimmune disease affecting lungs Condition
Being diagnosed with a rare autoimmune disease affecting lungs such as Hypersensitivity Pneumonitis (HP) or rheumatoid arthritis-associated lung disease requires adapting to a new normal focused on managing symptoms, preventing flares, and preserving quality of life.
1. Understanding Specific Conditions
Your journey may involve specific diagnoses like Hypersensitivity Pneumonitis, an immune-mediated lung inflammation caused by inhaling certain environmental antigens (e.g., mold, bird proteins). If your lung disease is linked to joint issues, you might also manage seronegative rheumatoid arthritis (RA without typical blood markers) or classic RA, coded in medical records as rheumatoid arthritis icd 10 (M06.9).
2. Core Management Strategies
The cornerstone of living well is a tailored treatment plan:
- For hypersensitivity pneumonitis treatment, the first and most critical step is antigen avoidance—identifying and completely removing the source (e.g., birds, moldy environments).
- Medical treatment often involves corticosteroids (like prednisone) to calm acute inflammation, and potentially long-term immunosuppressants (e.g., mycophenolate, azathioprine) to prevent progression.
- For RA-related lung disease, managing the systemic arthritis with DMARDs (Disease-Modifying Antirheumatic Drugs) or biologics is essential to protect the lungs.
3. When Advanced Interventions Are Needed
In severe cases where joints are severely damaged, rheumatoid arthritis surgery (such as joint replacement or synovectomy) may be recommended to restore function and reduce pain. Importantly, any surgery requires careful coordination between your rheumatologist, pulmonologist, and surgeon, as lung involvement can increase anesthesia risks.
4. Daily Life and Self-Care
Living successfully means embracing a holistic approach:
- Pulmonary Rehabilitation: A supervised program to improve endurance and breathing techniques.
- Infection Vigilance: Due to immunosuppressive medications, preventing illness through vaccination and hygiene is crucial.
- Support Systems: Connecting with patient advocacy groups for your specific condition can provide invaluable emotional support and practical advice.
The Path Forward
A proactive partnership with your medical team—typically a pulmonologist and rheumatologist—is your greatest asset. Through careful monitoring, medication adherence, lifestyle adjustments, and a strong support network, you can actively manage your health and maintain your daily life.